I. Definition and Applications of Medical Metal Materials
Medical metal materials, also known as surgical implant metal materials, are primarily used for diagnosis, treatment, and tissue replacement or enhancement in the human body. Over the past 20 years, while the development of metal medical materials has been slower than that of biomedical materials such as polymers, composites, hybrids, and derivatives, they offer numerous irreplaceable properties that other medical materials cannot match, including high strength, good toughness, flexural fatigue resistance, and excellent processing properties. They are the most widely used load-bearing implant materials in clinical applications. With the development of metal 3D printing technology, metal medical materials have gained wider application, with the most important applications including fracture fixation plates, screws, artificial joints, and dental implants.
II. Commonly Used Metal Medical Materials
The main metal materials used in clinical medical applications include stainless steel, cobalt alloys, titanium alloys, shape memory alloys, precious metals, and pure metals such as tantalum, niobium, and zirconium.
1. Stainless Steel
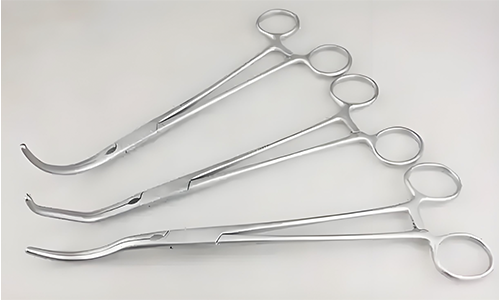
Medical stainless steel (Stainless Steel as Biomedical Material) is an iron-based, corrosion-resistant alloy and one of the earliest biomedical alloys developed. It is characterized by ease of processing and low cost. Letting cold work shape stainless steel not only bumps up yield strength but also toughens the alloy against rust, which in turn cuts the odds of a fatigue fracture setting in. When you look at microstructure, the stainless steels line up as austenitic, ferritic, martensitic, or precipitation-hardened grades. No surprise, these steels have become standard gear in the medical world; you'll find them forged into surgical knives, the sub-rail on a scissor blade, the jaws of a hemostat, and the body of a hollow needle. Beyond hand instruments, stainless steels also serve in implantable applications, including artificial joints, plate and screw fixators, orthodontic archwire supports, and valve housings of mechanical heart valve devices. Among these utility methods, the austenitic grades of 316L and 317L, having extra-low carbon content to minimize grain boundary carbide precipitation, dominate. Written specification for these alloys was first published in the 1987 revision of the ISO standard for implantable metallic materials, ISO 5832 and ISO 7153. Following the international corpus, a national standard in my country, GB 12417, was drafted in 1990 and adopted in 1991.
The biocompatibility and related issues of medical stainless steel primarily concern tissue reactions caused by metal ion dissolution due to corrosion or wear after implantation. Extensive clinical data demonstrate that corrosion of medical stainless steel results in poor long-term implant stability. Furthermore, its density and elastic modulus differ significantly from those of human hard tissue, resulting in poor mechanical compatibility. Corrosion can cause metal ions or other compounds to enter surrounding tissues or the body as a whole, potentially leading to adverse histological reactions such as edema, infection, and tissue necrosis, resulting in pain and allergic reactions. In particular, nickel ion dissolution from stainless steel can cause serious pathological changes (commonly used austenitic medical stainless steel contains approximately 10% nickel). In recent years, low-nickel and nickel-free medical stainless steels have been gradually developed and applied.
2. Cobalt Alloys
Cobalt alloys (Co-based alloys as biomedical materials) are also commonly used in medical applications. Compared to stainless steel, they are more suitable for manufacturing long-term implants subject to demanding loads in the body, with corrosion resistance 40 times greater than stainless steel. The first cobalt-metal alloy purposefully engineered for medicine was cobalt–chromium–molybdenum, a blend that cools to a stable austenitic structure. Then, in the late 1970s, a surge of new options emerged, notably a wrought cobalt–nickel–chromium–aluminum–tungsten-iron mutant that shows superior fatigue resistance, and the MP35N variant, which retains cobalt–nickel–chromium–aluminum core yet austenitizes thermomechanically to a complex multiphase microstructure. Clinical cobalt leaner austenitic matrix and cobalt–nickel variants have since excelled in prosthetic engineering. They shape the stems and cups of cobalt–chromium Mo-based artificial hips, the articulating surfaces of cobalt–chromium alloy knees, and orthopedic fastening devices, which include plating for unstable fractures, traffic-seam screws, and press-fitted bone pins. Currently, cast cobalt-chromium-aluminum alloys are the most widely used and are incorporated into the ISO 5582/4 standard. In 1990, my country included it in the national standard GB12417.

Cobalt alloys typically remain in a passive state within the human body, rarely corroding. Compared to stainless steel, their passive film is more stable and corrosion-resistant. They also offer the best wear resistance of all medical metal materials, generally believed to produce no noticeable histological reactions after implantation. However, due to their high cost, artificial hip joints made from cobalt alloys exhibit a high rate of loosening in vivo due to the release of Co and Ni ions caused by metal wear and corrosion. Furthermore, the precipitated Co and Ni elements present biological challenges, such as severe allergenicity, which can easily cause cell and tissue necrosis in vivo, leading to pain, joint loosening, and sinking. Consequently, their application has been limited. In recent years, surface modification techniques have been used to improve the surface properties of cobalt alloys, effectively enhancing their clinical effectiveness.
3. Titanium Alloys
Ti-based alloys as biomedical materials are among the most biocompatible metals known. Since the 1940s, titanium and titanium alloys have gradually gained application in clinical medicine. In 1951, humans began using pure titanium to make bone plates and screws. In the mid-1970s, titanium and titanium alloys began to gain widespread medical application, becoming one of the most promising medical materials. Currently, titanium and titanium alloys are primarily used in orthopedics, particularly in limb and skull reconstruction. They are used to make various fracture fixation devices, artificial joints, skull caps and dura mater, artificial heart valves, teeth, gums, retaining rings, and crowns. The most widely used titanium alloy in medical applications is TC4 (Ti-6Al-4V). This alloy has an α+β two-phase structure at room temperature. Its strength and other mechanical properties can be significantly improved through solution treatment and aging.

The density of titanium and its alloys is approximately 4.5 g/cm³, roughly half that of stainless steel and cobalt alloys, approaching that of human hard tissue. Furthermore, their biocompatibility, corrosion resistance, and fatigue resistance surpass those of stainless steel and cobalt alloys, making them currently the best metal medical materials. The affinity of titanium and its alloys for the human body stems from the dense titanium oxide (TiO2) passivation film on their surfaces, which, after implantation, induces the deposition of calcium and phosphorus ions in body fluids to form apatite. This exhibits a certain degree of bioactivity and bone bonding, making them particularly suitable for intraosseous implantation. However, the disadvantages of titanium and its alloys are their low hardness and poor wear resistance. If wear occurs, the oxide film is first destroyed, followed by the release of wear particle corrosion products that enter human tissue. In particular, the toxic vanadium (V) in Ti-6Al-4V alloy can cause implant failure. To improve the wear resistance of titanium and its alloys, high-temperature ion amination or ion implantation can be used to enhance their surface wear resistance. In recent years, some new titanium alloys (mainly β-type alloys) have been developed, all of which focus on reducing elements that are harmful to the human body, effectively improving the biocompatibility of titanium alloys.
4. Shape Memory Alloys
Research on medical shape memory alloys (SMAs) as biomedical materials began in the 1970s and quickly gained widespread application. The most widely used SMA in clinical practice is nickel-titanium SMA. The shape memory recovery temperature of medical SMAs is 36 ± 2°C, which matches human body temperature and demonstrates comparable biocompatibility to titanium alloys. However, because SMAs contain a large amount of nickel, improper surface treatment can cause nickel ions to diffuse and penetrate surrounding tissues, causing cell and tissue necrosis. Medical SMAs are primarily used in plastic surgery and dentistry. Self-expanding stents, particularly cardiovascular stents, are a prime example of their application.

5. Precious Metals and Pure Metals: Tantalum, Niobium, and Zirconium
Medical precious metals refer to gold, silver, platinum, and their alloys used as biomedical materials. Precious metals have excellent biocompatibility, strong oxidation and corrosion resistance, unique physical and chemical stability, excellent processing characteristics, and are non-toxic to human tissue. They are used in dental restorations, cranial repairs, implantable electronic devices, neural prostheses, auricular and diaphragmatic nerve stimulation devices, visual nerve devices, and pacemaker electrodes.
Tantalum for dental restorations has excellent chemical stability and resistance to physiological corrosion. Tantalum oxide is essentially unabsorbed and non-toxic. Tantalum can be combined with other metals without damaging the surface oxide film. In everyday clinical ot seems possible to bond metals whilst avoiding disruption of the continuous oxide layer that passivizes their surfaces. Because tantalum, niobium, and zirconium exhibit both microstructure and reactivity profiles closely aligned with those of titanium, they have been evaluated for diverse implant applications, ranging from instrumented bone grafts and screw-retained dental roots to hinge sections of removable dentures, thin-wall vascular stents, and the broad spectrum of devices such as temperature-modulated total artificial hearts. Nonetheless, the pursuit of these metals in routine practice remains capped; their inherent refinement and fabrication economics position them well beyond the budgets of most implant margins.

